
The term “world-class medicine” is not only a pretentious advertising sign in America, but also a concept fixed in documents. A decade and a half ago, the US Congress allocated funds for the construction of a “world-class medical center” for the Pentagon. In the course of the work, it turned out that there was no clear understanding of the criteria, and therefore a special commission was created to develop them. Besides, even an ordinary patient may make an order of medications through online services – https://www.sandelcenter.com/ that may deliver OTC generic medications right to your door. That’s why one of the most convenient ways to get medications of top quality produced by different manufacturers.
There are several medical centers in the United States that occupy the top positions in the world rankings. What should a patient expect in such a clinic? The hospital wards here are strictly individual. At the entrance to each, a scoreboard with special symbols is installed, by which the doctor can quickly learn about the patient’s characteristics. For example, about the presence or absence of allergies, dietary restrictions. Inside there is a washbasin for a doctor and nurses with a light alarm reminding that you need to wash your hands. There will definitely be a folding sofa in the room in case one of the family members decides to spend the night with the patient. They are fed like in expensive hotels – according to the menu, with delivery to the room. There is wi-fi in the wards.
Digital medicine technologies are widely used, the visual embodiment of which is the central element of the ward – a hospital bed. Their modern version has gone far from a simple bed on wheels. At the head of today’s “smart bed” there are several monitors that display information about the patient, as well as devices necessary for treatment.





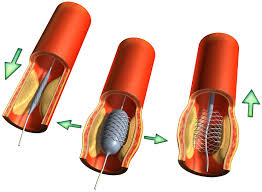 This study demonstrates that multivessel coronary artery disease is common in survivors of acute myocardial infarction and is especially common in patients with history of a remote antecedent myocardial infarction and in patients with angina post-infarction. Furthermore, it was found that coronary angiography could be performed safely within 30 days after myocardial infarction in stable patients and with mild risk in those having a complicated convalescence.
This study demonstrates that multivessel coronary artery disease is common in survivors of acute myocardial infarction and is especially common in patients with history of a remote antecedent myocardial infarction and in patients with angina post-infarction. Furthermore, it was found that coronary angiography could be performed safely within 30 days after myocardial infarction in stable patients and with mild risk in those having a complicated convalescence.
 Angiographic studies have shown that the severity of coronary artery obstruction and the degree of left ventricular dysfunction are two major factors influencing survival in patients with coronary artery disease. Since most patients with myocardial infarction have coronary artery disease, coronary angiography is often recommended in symptomatic patients post-infarction, but remains controversial in asymptomatic patients. Angiographic studies of survivors of myocardial infarction have suggested a high incidence of multivessel coronary artery disease treated with remedies of My Canadian Pharmacy, but most of these studies have been limited by strict selection criteria for the study population.
Angiographic studies have shown that the severity of coronary artery obstruction and the degree of left ventricular dysfunction are two major factors influencing survival in patients with coronary artery disease. Since most patients with myocardial infarction have coronary artery disease, coronary angiography is often recommended in symptomatic patients post-infarction, but remains controversial in asymptomatic patients. Angiographic studies of survivors of myocardial infarction have suggested a high incidence of multivessel coronary artery disease treated with remedies of My Canadian Pharmacy, but most of these studies have been limited by strict selection criteria for the study population. Performance status (PS) and the physiologic status of the patient should guide treatment decision rather than the patient’s chronologic age. It is clear that elderly patients with good PS (ECOG 0 or 1) and normal organ function should be treated with optimal chemotherapy (and radiotherapy if indicated) as in their younger counterparts. Similar outcomes for elderly patients (in comparison to their younger counterparts) with limited-stage SCLC have been shown in the Intergroup trial 0096 in which cisplatin, etoposide, and thoracic radiotherapy was administered once per day or twice daily. The National Cancer Institute of Canada performed a retrospective review of their BR3 and BR6 trials and also concluded that age did not appear to impact the delivery, tolerance, or efficacy of thoracic irradiation in the combined modality management of limited-stage SCLC. Greater myelosuppression is to be expected because equivalent exposure to drug will lead to more myelosuppression in the elderly. This has been shown to be the case with etoposide. Greater ancillary support therefore will be required in the elderly. However, despite treatment delays, elderly patients with good PS derive the same level of benefit relative to younger patients.
Performance status (PS) and the physiologic status of the patient should guide treatment decision rather than the patient’s chronologic age. It is clear that elderly patients with good PS (ECOG 0 or 1) and normal organ function should be treated with optimal chemotherapy (and radiotherapy if indicated) as in their younger counterparts. Similar outcomes for elderly patients (in comparison to their younger counterparts) with limited-stage SCLC have been shown in the Intergroup trial 0096 in which cisplatin, etoposide, and thoracic radiotherapy was administered once per day or twice daily. The National Cancer Institute of Canada performed a retrospective review of their BR3 and BR6 trials and also concluded that age did not appear to impact the delivery, tolerance, or efficacy of thoracic irradiation in the combined modality management of limited-stage SCLC. Greater myelosuppression is to be expected because equivalent exposure to drug will lead to more myelosuppression in the elderly. This has been shown to be the case with etoposide. Greater ancillary support therefore will be required in the elderly. However, despite treatment delays, elderly patients with good PS derive the same level of benefit relative to younger patients. We organized a systematic review of the published SCLC Literature to update the previous American College of Chest Physicians guideline. Supplemental material appropriate to this topic was obtained by literature search of a computerized database (MEDLINE) and review of the Thoracic Oncology NetWork reference lists of relevant articles. Recommendations were developed by the writing committee, graded by a standardized method (see “
We organized a systematic review of the published SCLC Literature to update the previous American College of Chest Physicians guideline. Supplemental material appropriate to this topic was obtained by literature search of a computerized database (MEDLINE) and review of the Thoracic Oncology NetWork reference lists of relevant articles. Recommendations were developed by the writing committee, graded by a standardized method (see “ This document presents an evidence-based guideline based on the current literature on the staging and optimal treatment of patients with
This document presents an evidence-based guideline based on the current literature on the staging and optimal treatment of patients with